Reports of wrong-site surgeries increased 62 percent in the past year in Connecticut hospitals, while the number of patient deaths or disabilities resulting from surgery or falls also rose, a new state report shows.At the same time, reports of patients suffering from serious pressure ulcers declined, as a number of hospitals made progress in preventing the painful bed sores.The new Adverse Event Report, compiled by the state Department of Public Health and covering 2011, marks the second year that acute-care hospitals and other medical facilities have been publicly identified by name, as they report errors that caused harm to patients.
The five hospitals with the highest rate of adverse events in 2011, calculated per 100,000 inpatient days, were: Charlotte Hungerford Hospital, in Torrington (49.2); Sharon Hospital (35.4); New Milford Hospital (32.9); Stamford Hospital (19.7); and the Hospital of Central Connecticut, in Southington and New Britain (19.3).
In terms of the sheer volume of events, Yale-New Haven and its affiliated Hospital of St. Raphael accounted for the highest numbers of errors – 21 each – while other large hospitals, such as Hartford and Danbury, also recorded more than 15 adverse events.
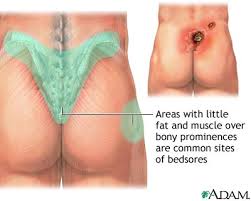
Reports of patients suffering from pressure sores declined last year, dropping to 39 – about half the number reported statewide in 2009. Hartford Hospital reported 3 cases, down from 20 in 2009, while Yale-New Haven reported 3, down from 13 in 2009. Eighteen of the state’s 30 acute-care hospitals reported no incidents of pressure ulcers.
Dr. Mary Reich Cooper, vice president and chief quality officer for the Connecticut Hospital Association, said the state’s hospitals are making extensive efforts to identify patients at risk of falls and pressure sores upon admission, and to reduce the likelihood of harm. Noting that the state has made progress in reducing hospital infection rates, she said the association is working with hospitals “to tackle these other issues” by sharing best practices and encouraging a team approach to safety.
In other areas, challenges remain. Reports of patients who had surgery performed on the wrong body part – an error which has been policed closely in recent years – increased from 8 in 2010 to 13 last year. Danbury, Greenwich, Hartford and St. Raphael’s hospitals each reported two such errors.
Before 2010, wrong-site surgeries were relatively rare in Connecticut – there were only two reported statewide in 2009.
Cooper said she believes hospitals have increased their reporting of all adverse events, so that more errors are being publicly disclosed. Although hospitals have adopted “checklists” and other measures to reduce wrong-site surgeries, those measures alone haven’t eradicated human error, she said.
“There’s a lot of focus right now on mindfulness. . . being mindful, instead of just going through the protocol,” she said. There is also an increasing emphasis on “a team approach” to preventing surgical errors, so that no one person is responsible for safety checks.
Reports of patient deaths or serious disability as a result of surgery rose from 16 incidents in 2010 to 21 last year. Five of the incidents were reported at Middlesex Hospital, but officials there said only one of the cases resulted in a death, while the other four were cases in which patients lost large amounts of blood but were not seriously harmed. Eight other hospitals reported one to three cases.
Perforations during open, laparoscopic and endoscopic procedures that resulted in death or serious disability remained high among hospitals, at 49 – up slightly from 2010. Bridgeport and Hartford hospitals each had six such cases.
Despite myriad efforts to reduce falls in hospitals, 96 patients died or were seriously injured from falling in 2011 – up from 91 the year before. Hospitals with the highest numbers of falls included Hungerford and Stamford hospitals, which each had nine cases. Hungerford also had a high rate of pressure ulcers.
Hungerford revamped its wound care program in 2009 to include “a more rigorous prevention and surveillance program” and is aggressively working to reduce falls, according to the hospital’s website.
Because errors are self-reported, state officials caution that some of the variation in rates could be due to underreporting. In July, a report by the U.S. Office of Inspector General found that many adverse events were not reported. In a representative sample of Medicare patients’ cases, 12 percent of the adverse events detected on chart reviews met state reporting requirements, but only 1 percent were actually reported, the study found.
The DPH adverse event report cautions: “Based on these data alone, we cannot derive certain conclusions. We cannot say whether a high. . . rate reflects highly complete reporting in a facility with good quality of care, or perhaps modestly complete reporting in a facility with poor care, or neither better nor worse quality care.”
The DPH reviews all hospital errors, but does not investigate every case. From Jan. 1, 2012, through Nov. 30, the department investigated about 27 percent of reported adverse events, according to DPH spokesman Bill Gerrish. From 2007 to 2010, about 23 percent of cases were investigated, last year’s report shows.
DPH officials said not every error warrants an investigation, and the agency targets instances where there is noncompliance with regulations or inadequate standards of care. The decision to investigate also is influenced by how often the type of event has been investigated before, and whether DPH is satisfied with a corrective plan that must be submitted by the hospital after an error is reported.
In the new report, DPH notes that in 2010, funding for part-time physician consultants to assist with case reviews was cut, hampering the department’s ability to conduct thorough investigations.
“The Department continues to feel that such specialized medical consultation enhances the comprehensive nature of the investigations, and is exploring alternative funding sources to revitalize this part of the process,” the report says.
In responses included in the report, most hospitals with high error rates described initiatives they were taking to reduce errors. Hartford Hospital touted its efforts to reduce serious falls and hospital-acquired pressure ulcers.
Stamford Hospital, which urged that adverse event reporting be viewed “in the context of the complexity of the patients cared for by the organization,” highlighted its efforts to reduce patient falls through a more detailed fall-risk assessment and targeted interventions for specialized patient populations.
A number of hospitals are participating in a “high reliability” program that seeks to create a culture of safety and make process changes to reduce accidents. At Middlesex Hospital, which reported no serious falls or pressure ulcers in 2011, Dr. Jesse Wagner, vice president for quality and safety, said the hospital had “ramped up” safety efforts in the last two to three years.
Middlesex has programs to identify patients at risk of falls and closely monitor their movements, and checks on patients’ skin conditions as soon as they arrive at the hospital, in order to assess the risks of developing bed sores, he said. Also, “many of our units are doing hourly rounding” to ensure that patients at risk of falls or sores are assisted, he said.
Danbury and New Milford Hospitals, members of the Western Connecticut Health Network, also said they had stepped-up efforts to reduce preventable harm in 2011 by implementing safety programs. The hospitals have an internal process for detecting “near-miss events,” officials said.
St. Francis Hospital and Medical Center has worked to reduce surgical errors, infections and falls, and has established a “non-punitive culture” for adverse event reporting, its response says.
None of the state’s ambulatory care centers reported more than three adverse incidents in 2011, and most of the reports concerned perforations during laparoscopic or other surgical procedures.
Among the centers, six reported rates higher than 45 incidents per 100,000 visits: The Coastal Digestive Care Center, in New London; Litchfield Hills Surgery Center, in Torrington; Hartford Surgical Center; Waterbury Outpatient Surgical Center; Digestive Disease Associates Endoscopy Suite, in Branford; and Leif O. Nordberg, MD, in Stamford.
To view the state’s adverse event report, click here.
Source: http://c-hit.org/2012/12/25/surgical-errors-climb-bed-sores-decline-in-states-hospitals/




